Abdulai, 26, helps his grandmother Beloca with basic physiotherapy exercises in their home. Photo: IOM/Monica Chiriac
In 2017, Tasnim was working as a medical officer in a maternity ward in Dhaka, where she helped deliver babies on a daily basis. When people started fleeing violence in neighboring Myanmar in 2017, Tasnim immediately joined a medical team which assessed an estimated 60,000 pregnant refugee women in Cox’s Bazar. After her weeklong assessment, and having experienced the chaos and realized the acute needs on the ground, she decided to stay. “I would have regretted not doing more,” Tasnim recounts.
Two years later, she started working as a programme manager with the International Organization for Migration (IOM)’s palliative care programme. IOM began strengthening palliative care services in the Rohingya refugee camps in early 2020, prior to the full-blown breakout of the COVID-19 pandemic and has since gradually integrated these essential services into the COVID-19 and healthcare general response.
Palliative care is a specialized medical field focused on providing relief for people living with a chronic or terminal illness, such as cancer, cardiovascular disease, stroke or paralysis. The goal is to improve the quality of life for both patients and caregivers.
“We focus on adding life to their days, not necessarily adding days to their lives,” Tasnim says. Research has shown that palliative care can not only improve the quality of life of patients with terminal illnesses, but in some cases, it can even improve their survival rate.

IOM’s small palliative care team in Cox’s Bazar sees up to 26 patients a day. Photo: IOM/Monica Chiriac
Tasnim’s new colleagues were convinced that it would be a long and painful transition for someone used to bringing life into the world. People were curious as to why a doctor like her would choose to work with people limited by disease instead of people with better prospects, she recalls. “I always need to remind people that we all die in the end, but the way we go matters. It matters to the people who are dying, and it matters to the ones around them.”
One of the pillars of palliative care deals with symptom management, providing direct pain relief for the patient’s physical symptoms. The second pillar focuses on delivering psychological support for both patients and caregivers to help them deal with the diagnosis and think about the next steps. “No one wants to talk about death or funerals, but sometimes we don’t know whether the patient has six days or six months to live and these are important discussions to be had,” Tasnim explains.
Regular referrals to IOM and partner Mental Health and Psychosocial Support (MHPSS) teams take place, while systematic anger management and emotional regulation training sessions are conducted for both patients and caregivers.
A terminal diagnosis has the potential to not only impact the patient but also their caregivers. For instance, the illness Khadija’s husband suffers from has left her anemic and depressed, but, through regular counseling sessions, her mood has gradually improved. As the longstanding primary bread winner in his family, her husband, 65-year-old Abdurahaman, now often feels like a burden.

As the longstanding primary breadwinner in his family, 65-year-old Abdurahaman now often feels like a burden. Photo: IOM/Monica Chiriac
What was a simple scratch on his foot seven years ago developed into an infection which eventually led to the amputation of three of his toes. But that didn’t bother Abdurahaman as much as he had anticipated. “I am ready to cut it all off if needed,” he says. Today, his diagnosis is peripheral artery disease with chronic kidney disease and hypertension. The medication, physiotherapy and psychosocial support have provided some much-needed relief for the entire family. “I can finally sleep at night,” Khadija says.
The team also tackles the topic of stigma that often accompanies the patient’s diagnosis, as most terminal illnesses are still perceived by the community as a curse from God. “We try to make them understand, at an individual level and the community one, that the illness is not their fault,” Tasnim says. Lastly, the teams work closely with spiritual leaders, who in turn support patients with the repentance process during their final days.

Since he started palliative care, 17-year-old Toha has regained sensation in his upper and lower limbs. Photo: IOM/Monica Chiriac
One of the team’s youngest patients is Toha, who, at barely 14, was shot in the neck as he was fleeing Myanmar with his family. His uncle and father had to carry him in a blanket all throughout the arduous journey to Bangladesh, where he was immediately rushed to the hospital. Not even extensive surgeries during the course of the next year could save Toha from quadriplegia.
Ever since starting palliative care, including symptom management, wound care, physiotherapy and psychosocial support, the now 17-year-old Toha has regained sensation in his limbs. “After almost three years, I can finally sit and move my hands,” he states. Although Toha will never fully recover from his injury, this small sign of independence has made a big difference in his life and that of his family.
Palliative care is still somewhat of a new field in Bangladesh, barely covered in the academic curriculum and with limited services across the country. “As doctors, we are always taught to focus on saving lives,” Tasnim says. At the national level, there are only three palliative care centres but none in Cox’s Bazar where there are currently 1.3 million refugees and host community members in need.
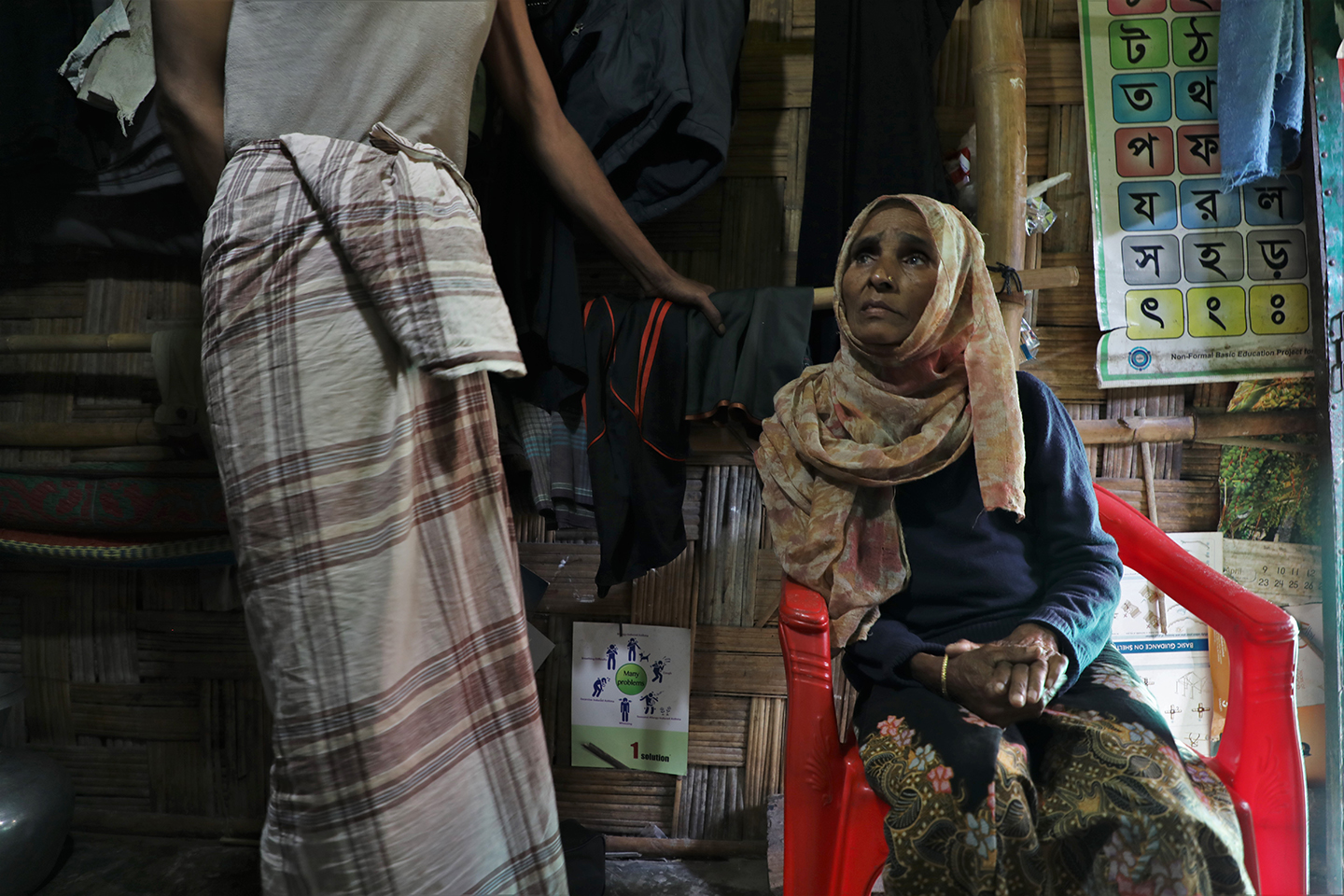
Since her stroke six months ago, Amina, 70, has been bedridden and unable to work. Photo: IOM/Monica Chiriac
Despite the growing recognition of the benefits of palliative care in humanitarian settings, its provision has largely been overlooked by the humanitarian sector. The palliative care team knows it is an uphill battle, but things are slowly changing, and palliative care is gradually becoming an established medical field in itself, less seen as spiritual healing or psychological support. Nowadays, the health packages at five IOM Primary Health Care Centres (PHCCs) in Ukhiya and Teknaf Upazilas (or sub-districts) in Cox’s Bazar include integrated palliative care as part of the services provided, while also offering house calls and community outreach activities.
If, back in 2017, when the palliative programme was first launched, people didn’t know or understand the term “palliative care”, nowadays, more and more people are reaching out for help. Furthermore, a variety of community groups are involved in the process and more referrals are taking place each day.
Notably, between December 2020 and January 2021, close to 800 patients received palliative care services, including pain and key symptom management, infection prevention, and referrals to appropriate teams for psychological and spiritual care. As of January 2021, 6,219 people have been reached by IOM’s community outreach teams raising awareness about palliative care and 7,888 inpatient/outpatient consultations have been conducted by the palliative care team.
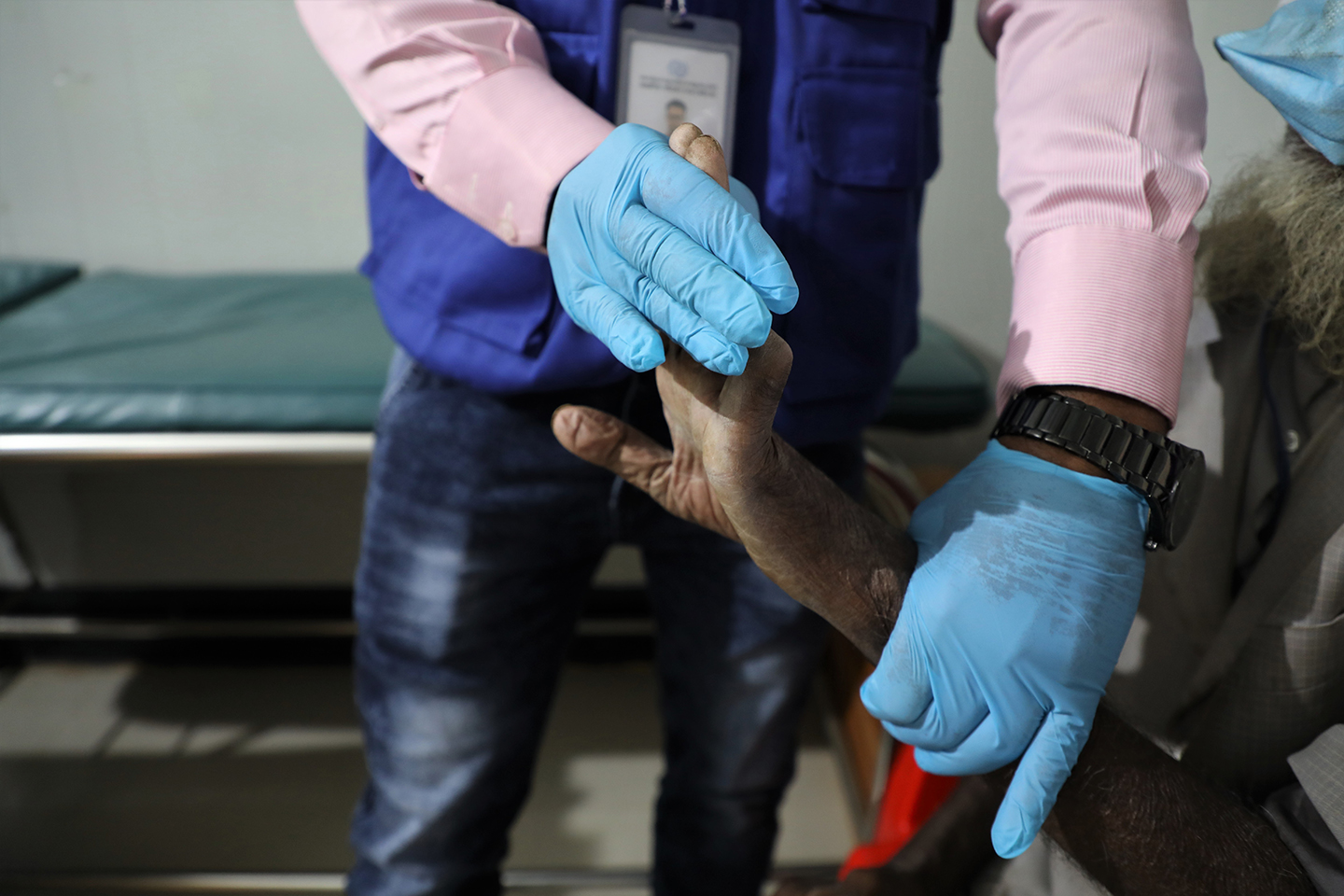
Jalal, 85, regularly comes to the clinic with his wife for his physiotherapy exercises. Photo: IOM/Monica Chiriac
The palliative care team may be small, but it regularly organizes capacity building activities for healthcare professionals and aims to scale up its activities to other health centres. Dr. Tawhid Mahmood, who has been working with the programme for almost a year now, recognizes the challenges of having such a small team: “We can’t always do house calls and not all the patients can come to the clinic on their own.”
The team’s objective is to empower families by teaching them how to perform caregiver-mediated exercises on their loved ones at home. Imam Hossain, the team’s physiotherapist, has taught Abdulai, 26, how to perform basic physiotherapeutic exercises for his bedridden grandmother Beloca.
Sixty-five-year-old Beloca had a stroke five years ago which rendered her hemiplegic. Since he learned the exercises six months ago, Abdulai has been performing them rigorously and devotedly. “I have definitely noticed an improvement since we started physiotherapy. Partial movement came back in her leg,” he says.

“We all die in the end, but the way we go matters. It matters to the people who are dying, and it matters to the ones around them.” – Tasnim. Photo: IOM/Monica Chiriac
Most caregivers and relatives are well aware of the fact that their loved one will sooner or later pass away – they just want them to have a respectful, dignified and pain-free life until then. Caregivers reach out to palliative care teams for support, who in turn go out of their way to ensure the patient’s end-of-life care is respected. “Families even get in touch after the patient dies to thank us for not abandoning them at the worst of times.” This only encourages the team to continue engaging in these difficult conversations with patients, caregivers and community members, but it surely doesn’t make the work any easier.
“At the end of the month, when I look back at what we did for the patient in their final days, it can be both rewarding and frustrating,” Tasnim says. “When I hear how much it means to people that someone cared about them when no one else would, it reminds me of the difference we are making.”
IOM’s palliative care programme in Cox’s Bazar is possible thanks to the support of the European Civil Protection and Humanitarian Aid Operations (ECHO), Australia’s Department of Foreign Affairs and Trade (DFAT), the Foreign, Commonwealth & Development Office (FDCO), and the World Bank.
For more information, please contact Monica Chiriac, Tel: +880 1880 084 048, Email: mchiriac@iom.int.


